
These intracranial-intracranial (IC-IC) bypass surgeries are simple, elegant, and more anatomic than their EC-IC counterparts. In recent years, innovative bypass surgeries have been introduced to revascularize the intracranial arteries with other intracranial arteries without extracranial donors. Moreover, the OA-PICA bypass has been used the most frequently as the EC-IC bypass based on the posterior circulation. Then, the superficial temporal artery to middle cerebral artery bypass is a standard treatment modality as one of extracranial-intracranial (EC-IC) bypass surgery. The revascularization is effective in occluding the aneurysm without risk of ischemic complications. Nevertheless, it causes such complications as lower cranial nerve dysfunction, potential injury to the VA and sigmoid sinus, increased incidence of cerebrospinal fluid leak, occipito-cervical instability and prolonged operation time 3, 4). In addition, far-lateral approach enables clinicians to achieve a proximal control and a lateral and parallel view along the axis of the vertebral and basilar arteries. Therefore, but it could be effectively resolved by trapping the aneurysms by far-lateral approach after occipital artery-posterior inferior cerebellar artery (OA-PICA) bypass surgery 9). Despite the excellent outcomes of trapping, it does not guarantee resolution of lateral medullary infarction 5, 6, 8). It has been proposed that a trapping of the lesion by far-lateral approach be performed to prevent subsequent rupture in patients with a dissecting aneurysm of the vertebral artery. This poses treatment challenges for clinicians with single standard treatment modality only. Because simple stenting method had still risk for rupture of aneurysm after intervention and parent artery occlusion had risk for ipsilateral PICA territory infarction, we decided that.Īs mentioned earlier, the dissecting vertebrobasilar aneurysms are one of the complex aneurysms. In this patient, we decided on the segmental occlusion using a coil with stent insertion of contralateral vertebral artery after PICA-to-PICA bypass surgery because of the proximity and parallel course of the distal segments of the PICA ( Fig. These findings were suggestive of a sign of impending rupture of left vertebral artery dissecting aneurysm because a short-term follow-up radiography revealed a change in the vessel contour. On day 10, the patient underwent transfemoral cerebral angiography (TFCA) showing complex vertebral dissecting aneurysm of long segment arising from the PICA ( Fig. 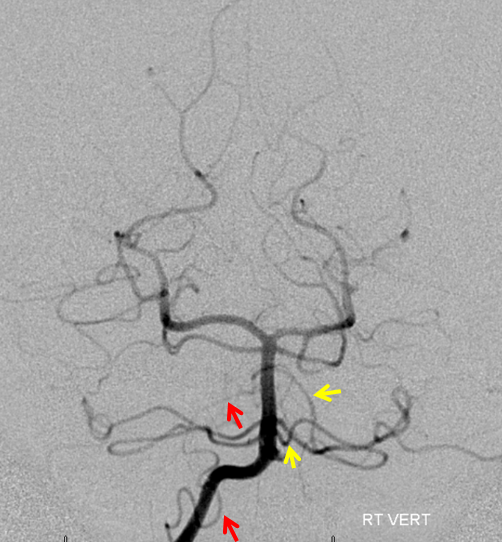
On day 5, the patient underwent magnetic resonance angiography at a follow-up, showing no interval change of left vertebral artery stenosis ( Fig. A 3-dimensional computed tomography angiography scan on admission showed left vertebral artery stenosis. On initial neurologic examinations, the patient had no neurologic signs. In conclusion our case suggests that the endovascular segmental occlusion of the parent artery followed by PICA to PICA bypass surgery through a midline suboccipital approach is a reasonable multimodal treatment option in patients with complex vertebral artery dissecting aneurysms.Ī 45-year-old woman was admitted to our hospital with a chief complaint headache and dizziness. At a 2-year follow-up, the patient achieved a good patency of both PICA. The aneurysmal sac was completely obliterated. This was followed by the endovascular segmental coil occlusion. Based on the aneurysmal morphology and the involvement of PICA, the patient underwent side to side anastomosis of the PICA. A 45-year-old woman has a left vertebral dissecting aneurysm with dizziness. Our case suggests that the endovascular segmental occlusion with posterior inferior cerebellar artery (PICA) to PICA side anastomosis might be a good treatment option in patients with complex vertebral artery dissecting aneurysms. We recently experienced a case of vertebral artery dissecting aneurysm and obtained good treatment outcomes. Treatment of complex aneurysms usually entails not only direct clipping but also alternative treatment modality.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
